Why Rosacea Keeps Coming Back — And What Changes When You Treat the Inflammation

Rosacea affects an estimated 16 million Americans. Most of them are being treated. Most of them are still dealing with recurrence.
The reason isn't treatment failure in the conventional sense. Topicals work. Antibiotics work. The skin improves, and then responds again, because nothing in that protocol addressed what was driving the inflammation in the first place. The cascade was quieted. It was never interrupted.
Understanding why rosacea recurs starts with the pathophysiology. And it ends with a treatment model built around mechanism, not visibility management.
The Inflammatory Cascade Behind Rosacea
Rosacea is a chronic inflammatory disease sustained by three reinforcing mechanisms.
Innate immune dysregulation. TLR2 is chronically overexpressed in rosacea-affected skin, triggering disproportionate cathelicidin production in response to UV, heat, and microbial triggers. Research in the Journal of Investigative Dermatology identified this immune overactivation as central to rosacea pathogenesis — reframing the condition as immune-driven rather than primarily vascular.1
Vascular hyperreactivity. Chronic immune activation drives neurovascular dysregulation: vessels dilate more readily, flush more frequently, and recover more slowly. A 2017 JAAD review confirmed that vascular hyperreactivity in rosacea is neurogenic and immune-mediated — which is why targeting vessels alone produces incomplete results.2
Barrier dysfunction. Chronic inflammation reduces ceramide production, increases transepidermal water loss, and lowers the skin's tolerance threshold — creating a loop where barrier breakdown increases reactivity to the triggers that cause inflammation.3
These mechanisms reinforce each other. Treating one without the others explains why rosacea so often recurs — and why recurrence is the expected outcome of suppression-based care, not a complication of it.
Where Conventional Treatments Fall Short
The limitations of standard rosacea therapies are failures of target selection, not efficacy.
Topicals — metronidazole, ivermectin, azelaic acid, brimonidine — reduce surface inflammation effectively but do not interrupt vascular reactivity or immune dysregulation at depth. Brimonidine's vasoconstriction produces fast visible improvement, but rebound vasodilation can worsen baseline redness over time. Many patients cannot tolerate formulations at all due to barrier compromise.
Oral doxycycline reduces inflammatory mediators and lesion count, but a randomized controlled trial in the Archives of Dermatology confirmed that benefit is sustained only with continued use — recurrence follows discontinuation reliably.4 It is a pause, not a solution.
Conventional laser and IPL platforms were designed for cosmetic vascular clearance, not inflammatory skin disease. IPL carries high epidermal thermal load — poorly tolerated in reactive rosacea skin and associated with PIH risk in Fitzpatrick IV–VI. For a full comparison of how Aerolase technology differs, see the technology overview.
Rosacea in Skin of Color — A Diagnostic and Treatment Gap
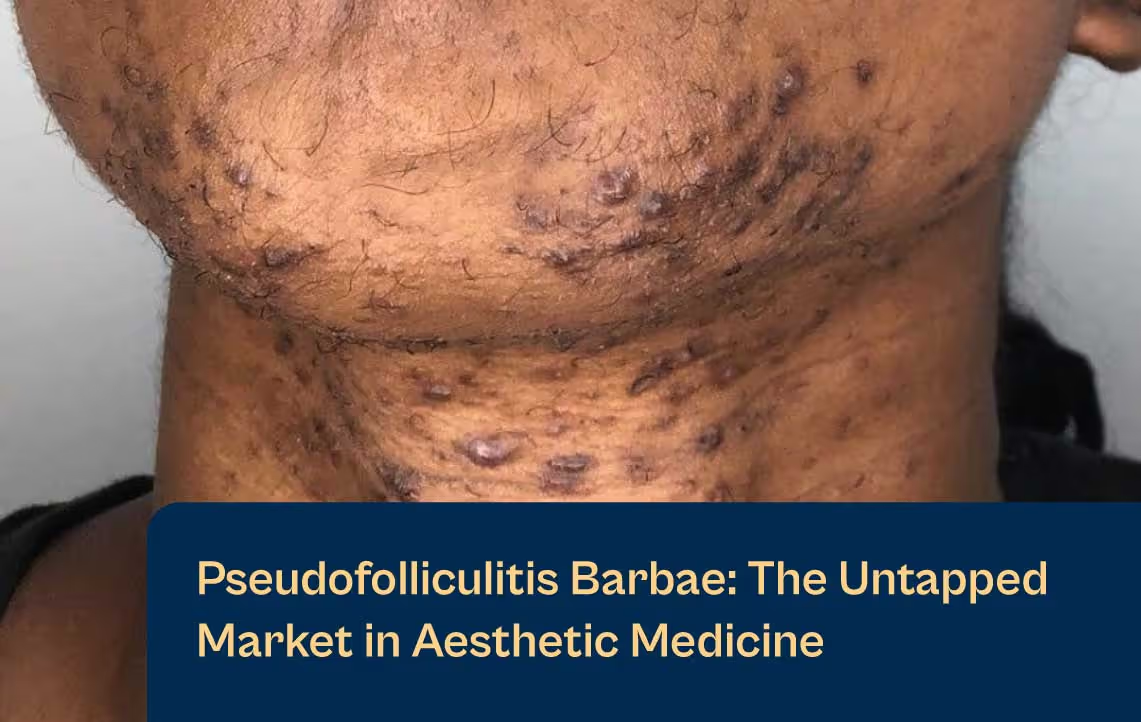
Rosacea in Fitzpatrick IV–VI is not rare, it’s underrecognized. A diagnostic model built around visible erythema in lighter skin types routinely misses the disease in patients of color, delaying treatment until inflammatory burden is significantly higher.
A landmark review co-authored by Dr. Valerie Callender confirmed that rosacea in skin of color is underreported due to diagnostic criteria that underweight clinical signs most apparent in darker skin.5 The consequences are measurable: delayed diagnosis, higher rates of phymatous progression, and a patient population arriving with more entrenched disease. Most conventional laser platforms compound the problem — PIH risk or outright contraindication in darker skin types leaves these patients underserved at both the diagnostic and treatment level.
Aerolase has published clinical data specifically addressing this gap — on rosacea-associated erythema and telangiectasias in skin of color treated with the 650-microsecond 1064nm Nd:YAG.
Read the case study, here.
The Inflammation-First Model — And How the Neo Elite Executes It
The inflammation-first approach reframes the clinical objective: the goal is not to quiet the skin, it's to reset how the skin responds. That requires intervening at the level of the cascade, not managing its visible output.
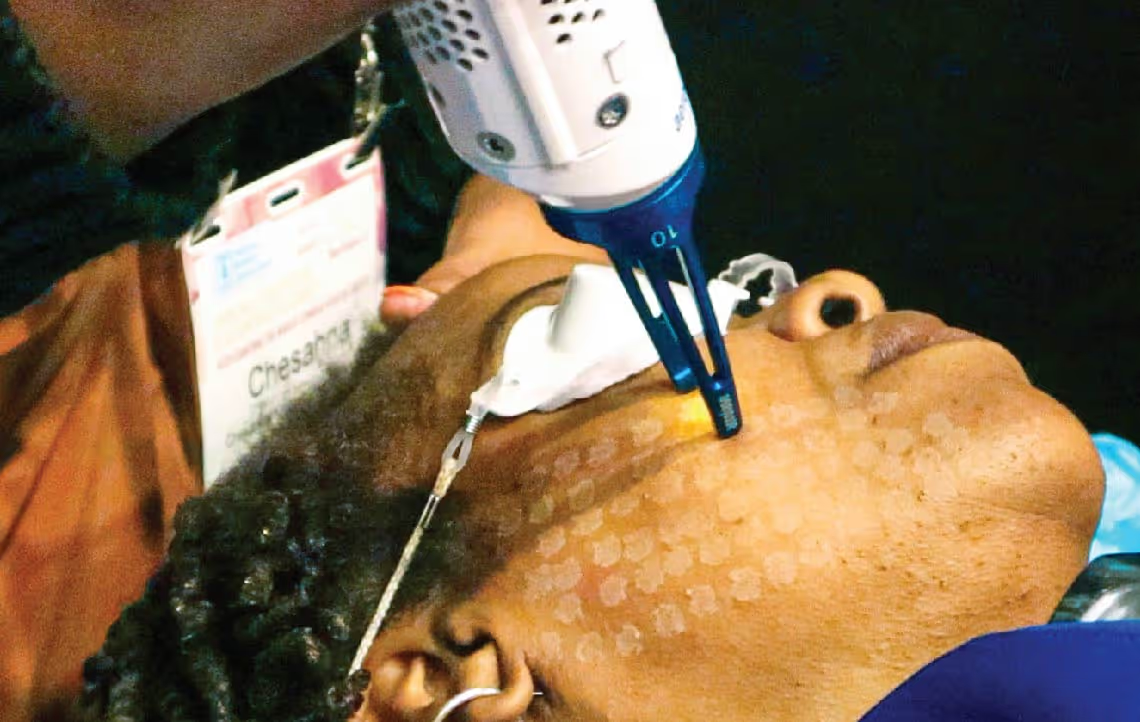
The Aerolase Neo Elite is a 1064nm Nd:YAG laser with a proprietary 650-microsecond pulse duration. The wavelength delivers deep dermal penetration with selective oxyhemoglobin absorption. The sub-millisecond pulse heats vascular and inflammatory targets at depth without transferring thermal energy to the epidermis — selective photothermolysis without the surface burden that limits other platforms.
Three simultaneous effects:
- Vascular targeting: Vessel collapse drives progressive reduction in erythema, flushing, and telangiectasia.
- Inflammatory modulation: Photothermal effect on mast cells and cytokines reduces papulopustular activity.
- Barrier support: Reduced thermal stress and collagen stimulation improve barrier integrity over time.
No cooling. No numbing. No downtime. Safe across Fitzpatrick I–VI. Published clinical evidence supports treatment of facial telangiectasias with the platform — see the full case review.
For the full clinical and indication overview, see rosacea, redness, and inflammation treatments at Aerolase, here.
Protocol at a Glance
Initial series: 4–6 treatments, every 2–3 weeks.
Maintenance: every 3–4 months based on severity and triggers.
Parameters (ETR/PPR): 28–36 J/cm², 7mm spot, 1–2 full-face passes — titrate conservatively on first session in reactive patients.
Combination sequencing: Neo Elite reduces the inflammatory baseline first — topical ivermectin, azelaic acid, barrier repair, and SPF layer in after establishing laser response. Avoid aggressive acids, retinoids, or ablative procedures during active flare.
The Bottom Line
Rosacea keeps coming back because the standard treatment model wasn't built to stop it. Suppressing visibility doesn't modify the vascular hyperreactivity, immune dysregulation, or barrier dysfunction sustaining the disease. Until treatment intervenes at that level, recurrence is the expected outcome — not a complication.
The inflammation-first model changes that. The mechanism explains it. The clinical evidence supports it. The patient outcomes confirm it.
To go deeper on the clinical framework, join us and Dr. Valerie Callender, President of the American Acne & Rosacea Society, for the webinar: Beyond Suppression: Rethinking Rosacea Through Inflammation.

Watch the full webinar, here.
Citations
- Yamasaki K, et al. Increased serine protease activity and cathelicidin promotes skin inflammation in rosacea. Nature Medicine. 2007.
- Steinhoff M, et al. Facial flushing and the vascular component of rosacea. JAAD. 2017.
- Two AM, et al. Rosacea: part I — pathogenesis and risk factors. JAAD. 2015.
- Del Rosso JQ, et al. Sub-antimicrobial dose doxycycline for rosacea. Archives of Dermatology. 2007.
- Alexis AF, Callender VD, et al. Global epidemiology and clinical spectrum of rosacea, highlighting skin of color. JAAD. 2019.